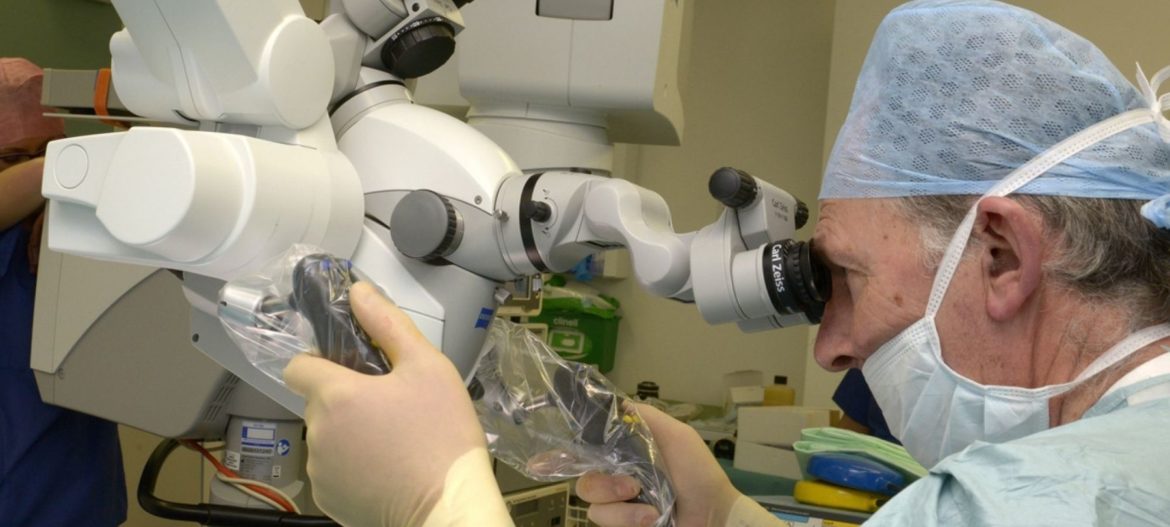
What is microdissection sperm retrieval?
When no obstruction of the testes is suspected (Non-Obstructive Azoospermia), the attempt to find and store sperm is more thorough, and involves the extraction of multiple small testicular specimens taken from different sites in each testicle. A microdissection sperm retrieval or a micro TESE and can only be undertaken using an operating microscope.
This surgical technique has been developed to detect sperm in the testicles of men who have poor sperm production.
Occasionally in non-obstructive azoospermia (NOA) non- surgical treatment may be effective, but this can only be expected in 10% of cases.
When the (non-obstructive) persists despite medical treatments, there are two options for the men: The traditional and accepted route is to suggest a ‘micro-TESE’ (testicular micro-dissection), or microsurgical testicular sperm extraction.
This important daycare procedure requires a light general anaesthetic and recovery is swift, but we recommend that men take one week away from work to ensure comfortable recovery, and to minimise complications.
The operation (m-TESE) requires a small (2 cm) cut on the front of the scrotum (sac). This incision is closed with stitches which are under the skin, and which dissolve without the need for removal or other post-operative care.
When the azoospermia is ‘obstructive’ (OA), a sperm retrieval procedure is inevitable, to allow sperm to be stored or used on the same day as the retrieval for IVF using Intracytoplasmic Sperm Injection (ICSI). Medical treatment is not helpful.
Sometimes, the sperm retrieval can be done without a general anaesthetic by percutaneous epididymal sperm aspiration (PESA). It is, however, more likely that we would advise a micro-epididymal sperm aspiration (MESA) under a light general anaesthetic, which gives the opportunity for reconstructive surgery, when it is possible and advisable to bypass an obstruction by a microsurgical epididymovasostomy. The MESA procedure (as opposed to the PESA) allows scope to extend the search for "best quality" sperm to the testicle itself, and also in our most recent practice to send the retrieved sperm for DNA fragmentation studies, to further refine our decision making when it comes to ICSI.
Even when obstructive azoospermia has been diagnosed, or is the likely diagnosis, we sometimes find that there are no motile, or normal, sperm in either of the epididymides and that therefore we need to proceed to a micro-TESE straight away, at the same time, and under the same general anaesthetic. It is therefore only the most ‘obvious’ cases of obstructive azoospermia in which we are ‘sure’ to find sperm in the epididymis, and when we are not proposing any other micro or reconstructive surgery, which are suitable for a PESA procedure under local anaesthesia.
The operative and post-operative descriptions and instructions are similar for both micro-TESE and MESA.
What about complications?
Fortunately there are very few with a microdissection sperm retrieval. Wherever an incision is made, infections under the skin (abscesses) and localised blood clots (haematomas, usually the size of a cherry) may occur. However, the incidence of such eventualities which either require treatment or which significantly alter the recovery trajectory are rare, occurring in less than 5% of all cases.
Are there any serious or long-lasting complications?
Much has been written about possible damage to the Testosterone-producing parts of the testicles. This sort of damage only occurs after a micro-TESE procedure, and not after a MESA, nor after epididymovasostomy, or vasectomy reversal.
The most favourable clinical reviews quote a 10% incidence of significant reduction in Testosterone production after micro-TESE. By ‘significant’, we mean that there is a need for Testosterone replacement therapy, because the damaged testicles cannot produce sufficient Testosterone for normal physiological functions.
The least favourable reviews quote incidences of low Testosterone (hypogonadism) in up to 25% of micro-TESE cases.
The real figure, in our experience, lies somewhere between the two; principally because the selective use of the FNA (mapping) procedure prior to micro-TESE means that we seldom need to operate on both testicles at the same time, thus preserving the hormonal (or endocrine) function at least one of the testes.
The risk of low Testosterone levels after micro-TESE is greatly increased when the micro-TESE has to be repeated. Therefore, when patients are seeking a second micro-TESE, or indeed a micro-TESE after previous multiple biopsies, we tend to offer a preliminary FNA mapping procedure, so that we will only be undertaking a micro-TESE when we know that sperm are present. It is rare in these cases to have to explore (and therefore potentially damage) both testes.
Finally, we may undertake a sperm retrieval (that is a micro epididymal sperm aspiration, or MESA) as part of a vasectomy reversal. The MESA adds very little time, and certainly no extra complications to the vasectomy reversal, and may help to indicate (by the quality and location of the sperm retrieved) what type of reconstruction might best suit the individual patient.
Recovery from vasectomy reversal operation (with or without a MESA procedure) often takes a little longer than from the other scrotal operation for sperm retrieval. Re-joining the vas tubes on both sides requires more dissection, and so the tissues in the scrotal sac and those surrounding the spermatic cords are necessarily more disturbed and will take more time to heal. The position of the testicles within the scrotal sac may also be altered.
Overall, we recommend 10 days off work, travelling and holidays following a reversal. Strenuous activity, including running and working out in the gym, should be avoided for at least one month post-operatively.